| Table of Contents |  |
|
Original Article
| ||||||
| Results of Wertheim-Meigs surgery for treatment of early uterine cervix cancer: An observational study | ||||||
| Karina Elord Castro Ribeiro da Silveira1, Claudio Sergio Batista2, Takasi Osako3, Claudia Lucia Nunes Alvares3 | ||||||
|
1MD, Faculty of Medicine of Petrópolis, Rio de Janeiro, Brazil.
2MD, MSc, PhD, Adjunct Professor of Gynecology & Obstetrics of Faculty of Medicine of Petropolis, Rio de Janeiro, Brazil. 3MD, UNIMED-Hospital, Petropolis, Rio de Janeiro, Brazil. | ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article |
| da Silveira KECR, Batista CS, Osako T, Alvares CLN. Results of Wertheim-Meigs surgery for treatment of early uterine cervix cancer: An observational study. Edorium J Gynecol Obstet 2016;2:8–16. |
|
Abstract
|
|
Aims:
To verify Wertheim-Meigs surgery outcomes for treating early uterine cervix cancer.
Methods: Observational, retrospective, not comparative study with cross-sectional data collection with 13 uterine cervical cancer patients stage IB to IIA undergoing to Wertheim-Meigs surgery from January 2000 to December 2012 in Petropolis, Rio de Janeiro, Brazil. Main outcomes were long disease-free, intraoperative and postoperative complications. Included variables were age, parity, sexual onset, number of partners, history of HPV infection, histological tumor type, status of surgical margins, lymph node involvement, and follow-up. Data were analyzed in PSPP software by calculating mean, median, and standard deviation. Results: Patients mean age was 43±13.20, parity 0.7±0.82 kids and sexual partners 3.54±3.55. White women were 69.30%, black 7.69% and other races 15.68%. Sexual onset mean was 15.98±5.75. Squamous cell carcinoma was 69.23%, adenocarcinoma 7.69% and adenocarcinoma of endometrium 15.38%. Lymph node commitment was 1 case. Intraoperative complications were bladder injury 15.38%, and a case of ureter section. Postoperative complications were intestine obstruction, cupola granuloma, and ureterovesical fistula a case each. Follow-up ranged from 1–7 years. Conclusion: Our study suggests despite of small sample it is need consider Wertheim-Meigs surgery as an efficient therapeutic option once the procedure presents good results and low complication rates. | |
|
Keywords:
Cervix uteri, Gynecologic surgical procedures, Hysterectomy, Uterine cervical neoplasms
| |
|
Introduction
| ||||||
|
Uterine cervix cancer is the third kind of female cancer worldwide [1], and every year there are about 4,800 fatal casualties and presents around of 18,340 new cases [2] [3]. More than 85% of the global burden occurs in developing countries [4] The main factor for uterine cervix cancer development is the human papillomavirus (HPV) infection, however, other factors may contribute for its carcinogenesis [5] [6]. Epidemiologically uterine cervix cancer is associated to early sexual onset, multiple sexual partners, low educational level, STD history, including chlamydial infection [7]. Initially, it is an oligosymptomatic or asymptomatic disease which leads many women to seek health service only when it is already in advanced stage, thereby reducing the chances of treatment and cure [8]. In disease evolving may arise episodes of nausea, vomiting, edema, lymphedema, intermittent vaginal bleeding, and after intercourse, vaginal secretions and abdominal pain, urinary and intestinal complaints at advanced cases [9]. The International Federation of Gynecology and Obstetrics establishes a standard staging for uterine cervix cancer (Table 1) whereas the stages IB and IIA as early, which can be treated by surgery or radiotherapy with high degree of success in both modes, while the stages of IIB to IV, advanced, have unfavorable prognosis [10]. According to Frederick, interest in developing surgical cure uterine cervix cancer predates the turn of 20th century, but despite these concerns, radical pelvic surgery showed excessive morbidity and mortality, thus the radiation treatment remained as choice for cervical cancer during the first half of 20th century, including reports of improvement in the survival of patients after the addition of pelvic lymphadenectomy to the radiation therapy [Taussig (1934, apud Frederick et al. 2011)], although some surgeons maintained the interest in improving surgical technique [11] as the inclusion of more extensive removal of parameters review and a complete pelvic lymphadenectomy proposed by Meigs [11] [12]. With regard to radical surgery complications, particularly fistulas, and its mortality these have been improved as the use of antibiotics and blood transfusions became more common [11]. In 1974, Piver et al., proposed a new classification for surgery for cervical cancer treatment in which establishes levels of surgical extension due to the different stages of the disease (Table 2), [11] [13] but classically uterine cervix cancer treatment has been divided into two groups, early stages (IA2, IB1, and small IIA with no parametrial involvement) and advanced stages (from IIB2 to IV) [14]. A new, simple and anatomy based classification of radical hysterectomy whose purpose was to preserve fertility, and, mainly, sympathetic and, parasympathetic innervation was described by Querleu and Morrow [15] and published in 2008, where they described four different types of surgery (Table 3). This study evaluated Wertheim-Meigs surgery for early uterine cervix cancer. The aim of the study was to verify Wertheim-Meigs surgery outcomes for treating early uterine cervix cancer. | ||||||
| ||||||
| ||||||
|
| ||||||
| ||||||
|
Materials and Methods
| ||||||
|
We carried out a longitudinal, observational, retrospective, descriptive and not comparative study, with cross-sectional data collection on which were included 13 patients undergoing to Wertheim-Meigs surgery for treating early uterine cervix cancer between 2000 to 2012 in Petropolis, a midsize highland city in the State of Rio de Janeiro, Brazil, as Public Health System, from Hospital Alcides Carneiro, as particular clinic from the surgeon that had performed the surgeries. Included patients were from both the public health system, Alcides Castro Hospital, as the private clinic of the surgeon who performed the surgery. It was included women whom had uterine cervix cancer stage IB to IIA by International Federation of Gynecology and Obstetrics (FIGO) 2009. It were excluded women with uterine cervical cancer stage less than IB or greater than IIA, that received prior treatment by radiotherapy or chemotherapy, those with uterine cervix cancer concomitant to pregnancy, and those cases operated by other surgeons. In this study, all patients were undergoing to surgical procedure by a unique surgeon in order to avoid the surgery execution bias, once it is a refined procedure and needs the same criteria of dissection in its execution, so all surgeries were performed by Wertheim-Meigs technic (Type III of Piver-Rutledge or Type C of Querleu-Morrow) Assessed outcomes were intraoperative and postoperative complications and long-disease free. Included variables were age, parity, sexual onset age, number of sexual partners, prior HPV infection history, histological tumor type, status of surgical margins, lymph node involvement and follow-up length. Data were analyzed in PSPP software for statistical analysis (GNU PSPP version 0.8.2) by calculating mean, median and standard deviation. This study is conformed to The Declaration of Helsinki and was approved by Faculty of Medicine of Petropolis Ethics Committee and registered under Certificate of Presentation for Ethical Consideration (CAAE – Certificado de Apresentação para Apreciação Ética) n° 24890614.6.0000.5245. | ||||||
|
Results | ||||||
|
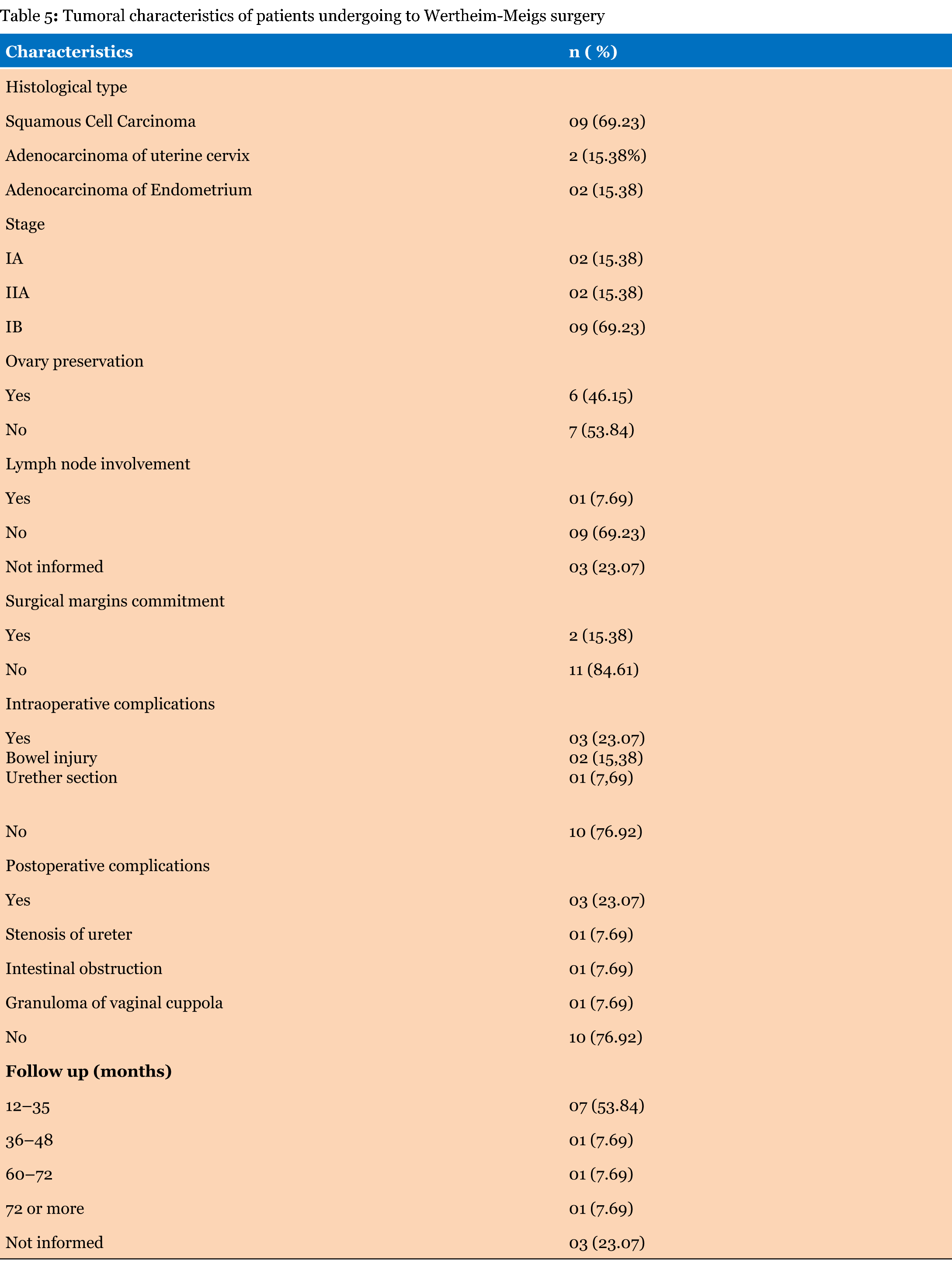
Patients age ranged 25–70 years (43±13.20), parity mean was of 0.7±0.82 kids/woman, mean of sexual partners was 3.54±3.55 per woman, white women were 9(69.30%), black was 1(7.69%) and other races were 3(15.68%), menarche ranged 10–17 years (12.92 ±1.71), sexual onset ranged 14–22 years (15.98±5.75), a patient reported never having had sexual intercourse and nobody mentioned neither HPV infection nor prior STD history. Regarding to type of tumor we found 9 (69.23%) squamous cell carcinoma of uterine cervix, 2 (15.38%) adenocarcinoma of uterine cervix and 2 (15.38%) adenocarcinoma of endometrium. About tumor stage 9 (69.23%) cases were IB and 2 (15.38%) were IA of uterine cervix cancer while other 2 (15.38%) were stage II A of endometrium carcinoma. Ovaries were preserved in 6 (46.15%) cases, lymph node and margins commitment occurred in 1 case and 2 cases, respectively. Intraoperative complications were bowel injury in 2 (15.38%) cases and urether section, a case, and postoperative complications were intestine obstruction, cupola granuloma, and ureterovesical fistula a case each. Ureter section had evolution to ureteral stenosis. Follow-up length ranged from 1 to 7 years and had no death consequent to uterine cervix cancer among all cases. Results have been summarized in Table 4 and Table 5. | ||||||
| ||||||
|
| ||||||
| ||||||
|
Discussion
| ||||||
|
This study shows the first results of an initial experience in surgical cervical cancer treatment from a gynecological surgery group in Petropolis, a midsize highland city of Rio de Janeiro, Brazil, whose goal is to promote medical care improvement in women who have uterine cervical cancer. We Consider as strong point of our work, despite the small sample, the fact that all patients have been operated by a single surgeon, thus eliminating both the patient selection bias as to procedure, since it is a very specific surgery by its nuances and that surgery should only be performed by a surgeon with appropriate expertise after careful patients evaluation. In other hand, we point as study limitation besides sample size the absence of information of tumor extension in pathology analyses which did us perform Wertheim-Meigs surgery (Type III of Piver-Rutledge or Type C of Querleu-Morrow) in all cases even though knowing that one has more complications than type I and II surgery [14] [16]. In spite of new surgical techniques for treating early uterine cervix cancer in use such as laparoscopy and robotic surgery, we believe that it is important to remember radical surgery for this condition since many places do not have support for these new approaches, and more and more women are at risk for this cancer whose mortality is still high. Factors influencing the decision to use surgery or definitive radiotherapy as the first treatment include patient factors (e.g., age, comorbidity, patient preference) and tumor factors (e.g., stage, tumor size, lymphovascular space invasion), as well as the physician's preference and resource availability [17], thus we just want bring the issue about treatment available at the time of cervical cancer diagnostic for discussion why maybe the Wertheim-Meigs surgery is the only one possible, but can be overlooked in name of most modern treatments but which are not available or feasible in certain regions such as ours. According some authors, there is no standard management of stage Ib to IIa cervical carcinoma and most often, stage Ib1 cervical cancer is treated by radical hysterectomy with pelvic lymphadenectomy [18]. However it has been showed that extra-fascial hysterectomy is generally considered adequate treatment for stage Ia1 cervical cancer type 2 modified radical hysterectomy with pelvic lymphadenectomy is usually used for stage Ia2 cervical cancer [11] [19]and type 3 radical hysterectomy with pelvic and para-aortic lymphadenectomy is used for patients with stage Ib and IIa cervical cancer [11]. Many gynecologic oncologists are in favor non-operative treatment in elderly patients and 65 years of age is frequently cited as the limit for consideration of radical hysterectomy. However, other authors have found that the morbidity and survival of older patients is comparable with that of younger patients [20] [21]. It was included in this series a 70-year-old patient and it was observed similar evolution to that of younger patients. Intraoperative and postoperative complication rates are 4% and 12%, respectively. Ten percent of patients had indications for adjuvant treatments. The risk of recurrence is statistically higher for those with tumor sizes >2 cm and LVSI [22] Intraoperatively, the most common complication of radical hysterectomy is hemorrhage; the range of reported average blood loss is from 600 mL to 1900 mL [23] [24] [25] but in this study there was no significative bleeding or need of blood transfusion. Complications that arise during the postoperative period include both early and late complications. Early complications are those occurring within the first 30 postoperative days, may vary [11]. It has been reported that up to 40% of early cervical cancers are diagnosed in young women [26] and our study showed 46.15% of cases ranging from 25 to 40 years. In this study, all cases were uterine cervix cancer stage IB and adenocarcinoma of endometrium stage IIA in according to literature which establish two treatment options such as primary surgery or chemo-radiotherapy depending on the individual characteristics, co-morbidities and preferences [18] [27]. Although most uterine cervix cancer are squamous cell carcinomas, the incidence of such carcinomas has declined over time, and cervical adenocarcinoma has risen in recent years, and human papillomavirus (HPV) infection and others cofactors may explain this differential trend is unclear [28] and although our results showed prevalence of squamous cell carcinoma we had no evidence of HPV infection neither on cancer diagnosis nor as prior STD infection. Regarding to lymph nodes spread this is common and usually occurs in a stepwise fashion, first to pelvic lymph nodes and then to para-aortic nodes. It is estimated that 15% of stage I, 30% of stage II, and 45% of stage III patients have pelvic nodal disease [22] [29]. We had only 01(7.69%) pelvic lymph nodes commitment. Complications in radical surgery seen in our work are in according to what has been showed in literature [11] and are at acceptable levels however we do not are able to affirm the range of complications would be the same if we had had more cases. | ||||||
|
Conclusion
| ||||||
|
Despite our small sample and although there are new procedures for treatment of early uterine cervical cancer it is necessary to consider the surgery of Wertheim-Meigs as efficient therapeutic option and our study suggets it provides good results and an acceptable complications rates. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions:
Karina Elord Castro Ribeiro da Silveira – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Final approval of the version to be published Claudio Sergio Batista – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published Takasi Osako – Acquisition of data, Revising it critically for important intellectual content, Final approval of the version to be published Claudia Lucia Nunes Alvares – Acquisition of data, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2016 Karina Elord Castro Ribeiro da Silveira et al. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|